All Posts in Category:Original Article
Yoga share
 Yoga is good for the body AND the mind. In addition to the obvious health benefits of regular exercise, a good yoga instructor creates an environment that promotes:
Yoga is good for the body AND the mind. In addition to the obvious health benefits of regular exercise, a good yoga instructor creates an environment that promotes:
- A sense of serenity and acceptance for who you are in the moment.
- Guidance for how you can recognize when your “monkey mind” is swinging from thought to thought with the worries of the day and gently turn your attention back to the present moment and the feeling of your nourishing breath
- Feeling comfortable in your own skin.
- Increasing confidence as your strength and flexibility grows.
There is a TON of research that strongly supports using yoga to assist with the treatment of: anxiety (including Post Traumatic Stress Disorder); depression; ADHD; sleep problems; substance abuse, anger issues, and schizophrenia (when done in conjunction with medication). It’s an activity that can be modified for people of any age, from 2 to 102, and you can take with you anywhere you go! There are even some instructors that have training in both mental health therapy and yoga and can customize the work to really target anxiety and trauma specifically, teaching you how to be comfortable in your own body again.
Personally, my ability to use relaxation breathing as a skill in my daily life has never left me, even though I haven’t done a class for almost 10 years. One day, when my life gets a bit simpler, I fully intend to return to the benefits of a more regular, devoted yoga practice. In the meantime, I remind myself the words of wisdom of one of my former instructors, “Even one sun salutation is a yoga practice.”
More Resources for Parents of People with Addiction share
 This month there is a very interesting article in Money Magazine, These Parents are Cutting Off Their Opioid Addicted Children: And it’s the Toughest Decision of their Lives by Kristen Bahler. It speaks to the very difficult choice many parents in this position face, financially. As with everything else, there is no singular path that people should follow in every situation. However , a lot of parents eventually come to a point where, partial, or even complete, withdrawal of financial support ultimately is the “right” answer.
This month there is a very interesting article in Money Magazine, These Parents are Cutting Off Their Opioid Addicted Children: And it’s the Toughest Decision of their Lives by Kristen Bahler. It speaks to the very difficult choice many parents in this position face, financially. As with everything else, there is no singular path that people should follow in every situation. However , a lot of parents eventually come to a point where, partial, or even complete, withdrawal of financial support ultimately is the “right” answer.
My training in substance abuse is limited, so I don’t recommend that you consider taking these steps without consulting with a substance abuse professional. Nevertheless, because of the pervasiveness of addiction in our culture, I still find myself working with people around these issues. It’s a tricky issue for parents and I can completely relate to the temptation to try to do what initially feels like being the most supportive parent you can be and then ultimately realizing that you are enabling your child’s unhealthy choices and behavior. I think it’s a normal process that most go through until they find a balance of what’s right for them.
One thing I will say, overall…I definitely recommend that setting financial boundaries, as well as personal ones, work best when framed in a firm yet loving/accepting way. This is a hard skill to learn. Therapists and support groups can provide guidance about how to do this. I also really like the CRAFT program, which I have written about, previously. The main reason I make this recommendation actually isn’t for the parents’ benefit, it’s for the addicted family member. It’s easier for people to step onto the challenging path towards recovery when they know that your love is, and will always be, there for them. Shame and humiliation only serves to make people feel worse about themselves and gives them more reason to avoid their feelings with intoxication. You have to walk the line of loving acceptance and logical boundaries. Remember, love doesn’t mean doing everything they expect of you.
There is one critical detail that I think a lot of parents, and even some professionals, overlook when parents are stuck in rescue mode. It’s important to understand that there is a subtle message that is communicated when we repeatedly bail out our kids, “I don’t think you are capable of solving this problem or even figuring out how to attempt to solve this problem,” and, “It’s my job to protect you from all of life’s stresses and discomforts.” The biggest problem with this underlying message is that everyone’s life involves being able to tolerate discomfort and solve problems. These are core life-skills that we all need to learn, one way or another, and the only way to do this is through uncomfortable experience, making mistakes, and becoming more skilled over time. This taps into my favorite thing to teach people about, having a Growth Mindset. I encourage you to check it out.
Getting back to the Money article, there are several resources listed that can be helpful to parents. I will link them here for your convenience.
- Parents of Addicted Loved Ones (PAL) – a faith-based network of parent-volunteer run support groups, including two weekly telephone groups if there isn’t an in-person group close to you. They have a specific, education driven series of presentations, and these resources are available on their website.
- Learn to Cope – online forum for family members of addicted loved ones.
- Substance Abuse and Mental Health Services Administration (SAMHSA) – a government website that, among tons of information and resources, includes several different 24/7 information and treatment referral hotlines.
- Al-Anon & Nar-Anon – volunteer, peer-run groups focusing on educating and supporting loved ones affected by addiction. Based on the 12-step model used by Alcoholics Anonymous/Narcotics Anonymous.
- Grief Recovery After Substance Passing – a community of support groups who have lost loved ones to addiction and overdoses.
Stages of Change share
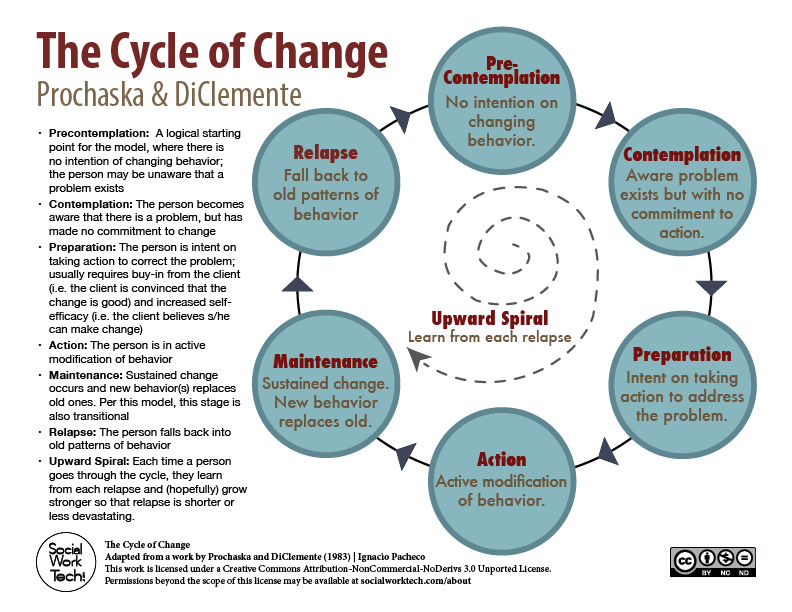
Once upon a time there were two researchers, Prochaska & DiClemente. (If you can’t already tell, I’m in a bit of a silly mood at the moment.) They were smart people who did research and read other people’s research and put it all together back in 1983 to come up with their Stages of Change model. This model is used heavily in the treatment of addictions but can also be applied to things like the treatment of anxiety and depression…or almost anything really, where change is involved. What they so wisely realized, when it came to making a change in one’s life, was that in addition to understanding the human mind and what can help it to change, you also need to be aware of the person’s readiness to actually do the work to make the change that they are looking for. The stages are Pre-Contemplation (when you don’t even have the desire to make a change), Contemplation (when you recognize that there is a problem and you are starting to consider if you want to make a change), Preparation (when you are starting to gather the resources and information you might need to help you make this change), Action (actively working on making the change happen), and Maintenance (you’ve made the change and can finally start to not work so hard on it, but there may still be some things you need to do to keep this positive change in place).
The Stages of Change model can help us to be patient with ourselves. It can help us to recognize how really ready we (or someone we care about) might actually be to make a significant change in our life. And, it can help us to realize what steps we can take to get ourselves closer to being ready to make this change. There is a therapeutic approach, Motivational Interviewing, that is also heavily rooted in the treatment of addictions but that can be applied in all sorts of other places. Motivational Interviewing is a technique that helps therapists, parents, even friends, to be accepting of the stage of change that a person is in at this moment, and being able to work with them (rather than battle with them) to explore small steps that they might feel comfortable with doing that will get them closer to being ready for change. (I plan to make a post on that at some point but for now, I leave you with doing an internet search.)
Below is an illustration of these stages. I like this illustration in particular because it’s drawn with a spiral rather than in a linear way. This is because there are no rules about the actual order we need to go in as we head towards change. And, sometimes, we even go backwards to an “earlier” level.
Panic Attacks Part 1: What is Panic & Why We Need It share
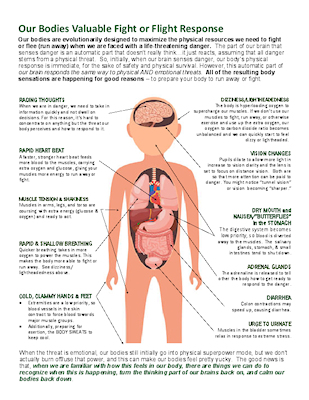
Panic is a normal, necessary physical response to the brain perceiving a significant threat. It involves the release of a hormone that you are likely familiar with, adrenaline. Adrenaline’s job is to tell the body to make chemical changes in the body so that the body is physically primed to either fight or flee/run away, from the threat. These can be things such as:
- Rapid heartbeat
- Short, shallow breaths
- Paling or flushing (can switch between both)
- Digestion slows down or stops (becomes a low priority for your body)
- Constriction of blood vessels in many parts of the body…including the BRAIN (which interferes with your ability to think logically)
- Dilation of blood vessels for muscles (so they are ready for action)
- Take energy from stored nutrients to fuel muscles
- Dilation of pupils
- Temporary loss of hearing
- Tunnel vision (loss of peripheral vision)
- Physical shaking

Back in the day of the caveman, the people who didn’t have a panic response were much less likely to survive because their bodies were not as prepared to deal with a physical threat. Our body’s ability to quickly maximize all of our resources for survival is a critical aspect not only of humans but all animal species. Yet, in our Western culture, many of us are fortunate that our safety is not regularly threatened in a physical way. Instead, because our brain does not recognize a difference between a physical threat and emotional threat, in a modern society a panic response can often be triggered by things such as fear of embarrassment or fear that a bridge might collapse. Or, perhaps you do have experience with your physical safety being at risk and now, your body is in hyper-vigilant mode and looking for danger at every corner.
The problem here is that our body’s physical readiness to fight or run won’t help us to not be embarrassed. Nor will it help us cross a perfectly well-maintained bridge or walk around the corner in a typically safe neighborhood. Instead, that physical response can feel scary itself and physically uncomfortable if we don’t do anything to burn off that energy and bring our body back to calm. Additionally, increasing our breathing rate without making use of the extra oxygen we are taking in creates a chemical imbalance between the oxygen and carbon dioxide levels of our body that adds to our feelings of physical discomfort.
So, what can we do if we start to physically panic about a possible emotional threat? Check out the next article in this series!
Remaining articles in this series:
- Panic Attacks Part 2: The Antidote to Panic – Relaxation Breathing
- Panic Attacks Part 3: Fear of the Fear – Don’t Let Panic Attacks Take Over Your Life
- Panic Attacks Part 4: Time To Tune Into Your Early Warning System (coming soon)
Panic Attacks Part 2: The Antidote to Panic - Relaxation Breathing share
Previous article in this series:
- Panic Attacks Part 1: What is Panic & Why We Need It
Relaxation breathing is the antidote to panic. Literally. It is impossible to be truly breathing in a relaxed way and to be experiencing a full-blown panic attack at the same time. This is because relaxation breathing helps to reset our body chemistry to a “normal” state and bring it out of panic. If you haven’t read it yet, the previous article in this series, Panic Attacks Part 1: What is Panic & Why We Need It, you might want to check it out.
Some people may tell you that there is a “right way” to do relaxation breathing. In my opinion, if you try the “right way” and you find it to be really annoying and just plain won’t do it, then clearly that is not the right way for you. Generally, the recommendation is that you are breathing out for a longer count than you are breathing in and that you are taking in air by expanding your belly muscles, not your chest muscles.
My recommendation is that you find something that feels comfortable for you and go with that approach. No matter which approach you choose, the most important thing is that you practice relaxation breathing every day when you are already calm. I cannot stress this point enough. When your body is in panic mode, learning a new skill is not something that your brain is going to be very good at. So if you’re heading into a panic attack and you haven’t been practicing your relaxation breathing, don’t be surprised if it doesn’t work to help you return to calm…yet.
Regardless of the breathing technique that you decide to use, I recommend that you practice your relaxation breathing during a time that you are already relatively calm and relaxed, for five minutes at a time, a minimum of 1-2 times every day, with one of those times being at night when you are lying down to fall asleep. The main goal is to be able to clear your mind of all thought and just focus on the sensation of your breath going in and out of your body. Or, you can add some sort of positive phrase that you can repeat to yourself if it helps. (For example: “Breathe in calm. Breathe out fear,” but it could be anything so long as you interpret it as positive and relaxing.)
Below is a video that describes square breathing and then, below that, a few other informational links. The video is geared towards kids but you can use whatever imagery you like, and, who doesn’t enjoy the smell of fresh baked cookies?? (You’ll understand that last comment when you watch the video.)
Additional Breathing Information:
- Another take on square breathing, including a printable that you can download and customize.
- Diaphragmatic breathing, also known as “belly breathing,” which can be blended with square breathing if you’d like.
If you have a smart phone, there are also plenty of free apps that you can download to help coach you through relaxation breathing. Here are two that I’ve had experience with:
- Breathe2Relax – availabe on iPhone and Android (I recommend adjusting the default settings to what is comfortable for you.)
- Centered – available on iPhone only 🙁
Remaining articles in this series:
- Panic Attacks Part 3: Fear of the Fear – Don’t Let Panic Attacks Take Over Your Life
- Panic Attacks Part 4: Time To Tune Into Your Early Warning System (coming soon)
Panic Attacks Part 3: Fear of the Fear - Don't Let Panic Attacks Take Over Your Life share
Previous articles in this series:
- Panic Attacks Part 1: What is Panic & Why We Need It
- Panic Attacks Part 2: The Antidote for Panic & Relaxation Breathing
Panic attacks feel very intense when you have them. At best, it’s not a comfortable feeling. At worst, it feels very scary because your body feels like it’s out of control. Some people even worry that they are having a heart attack. If you are experiencing these symptoms for the first time, definitely talk with a medical professional to rule out any medical causes before treating the symptoms as a panic attack. This is important for two reasons. The first is that you need to get a proper diagnosis. The second is that if you are constantly worrying that you are having a heart attack…that’s going to increase your anxiety and make successfully treating panic very difficult.
 Once you know that your body is healthy and ok, it’s time to dig in to the emotional aspects that come into play with panic and anxiety. When you worry too much about the possibility that you might have a panic attack, then this worry itself can become the trigger for your next panic attack. I call this having “fear of the fear (that it will happen again).” With the use of acceptance, information, “growth mindset,” and skill development, here are some guidelines that work against the negative spiral that can happen when people start to develop a “fear of the fear.” This article assumes that you already have started working on developing the skills for turning around a panic attack and is part 3 of a four-part series of articles I hope to complete. Hopefully, I’ll get part 4 up soon!
Once you know that your body is healthy and ok, it’s time to dig in to the emotional aspects that come into play with panic and anxiety. When you worry too much about the possibility that you might have a panic attack, then this worry itself can become the trigger for your next panic attack. I call this having “fear of the fear (that it will happen again).” With the use of acceptance, information, “growth mindset,” and skill development, here are some guidelines that work against the negative spiral that can happen when people start to develop a “fear of the fear.” This article assumes that you already have started working on developing the skills for turning around a panic attack and is part 3 of a four-part series of articles I hope to complete. Hopefully, I’ll get part 4 up soon!
- Recognize that this is a new situation for you and, because of that, it makes sense that it’s hard in the beginning to figure out what’s happening and how best to manage it. Also, know that you’re not alone. There are many people who have or are currently going through this too.You are having, what is called, a panic attack. [Growth Mindset]
- Remember that fight or flight mode is a normal thing that our bodies do. The only problem is that it’s getting triggered when you don’t actually need to respond physically to an emotionally stressful situation. The most important thing to know here is, NO HARM WILL COME TO YOUR BODY AS YOU EXPERIENCE IT (your body physically revving up to fight or flee). It does feel yucky to be in physical panic mode. This is especially true because your body, in that moment, is primed with an abundance of energy to physically react and that means that you experience temporary physical changes to your body (i.e. increased heart rate, quick & shallow breathing, increased blood circulation to muscles, decreased blood circulation to the “rational” part of your brain, and more), but your body naturally knows how to shift out of this mode when the perception of a physical threat is gone. [Watch this great video about how the US government has learned to train Navy SEALS not to panic.]
- Accept that this is not your last panic attack. What I’m saying here is find a way to be ok with knowing that it will happen again AND that should one happen and your growing relaxation and cognitive skills can’t turn it around, you can ride it out until it’s done and be still be ok. In general, the goal is for the panic attacks to start reducing in intensity as you get better at turning them around but this won’t happen if you avoid panic attacks, or things that might cause them, rather than face them. [Acceptance]
- Continue to experiment with and practice various relaxation techniques (relaxation breathing is the most important one for panic) and good self care habits so that you can hone your skills and have more “tools” in your “toolbox” when the need arises. [Skill Development]
- Work on developing cognitive strategies that can help prevent panic attacks from happening or intervene at the early signs of panic so that you can prevent a full blown physical response. [Skill Development]
- Keep a list of things that help turn your panic attacks around so that you can refer to the list the next time. [Skill Development]
- Remembering that low blood sugar, hypoglycemia, can mimic the beginning feelings of a panic attack, carry a healthy snack with you that has a nice combination of protein and complex carbs. [Check out this podcast by Dr. Kristen Allot about why this is so incredibly important.]
- Minimize or, ideally, eliminate caffeine. Drink water. Enjoy water. Did I mention water? [Information]
Remaining article in this series:
- Panic Attacks Part 4: Time To Tune Into Your Early Warning System (coming soon)
An Overview of the Range of Mental Health Services for Children and Adolescents share
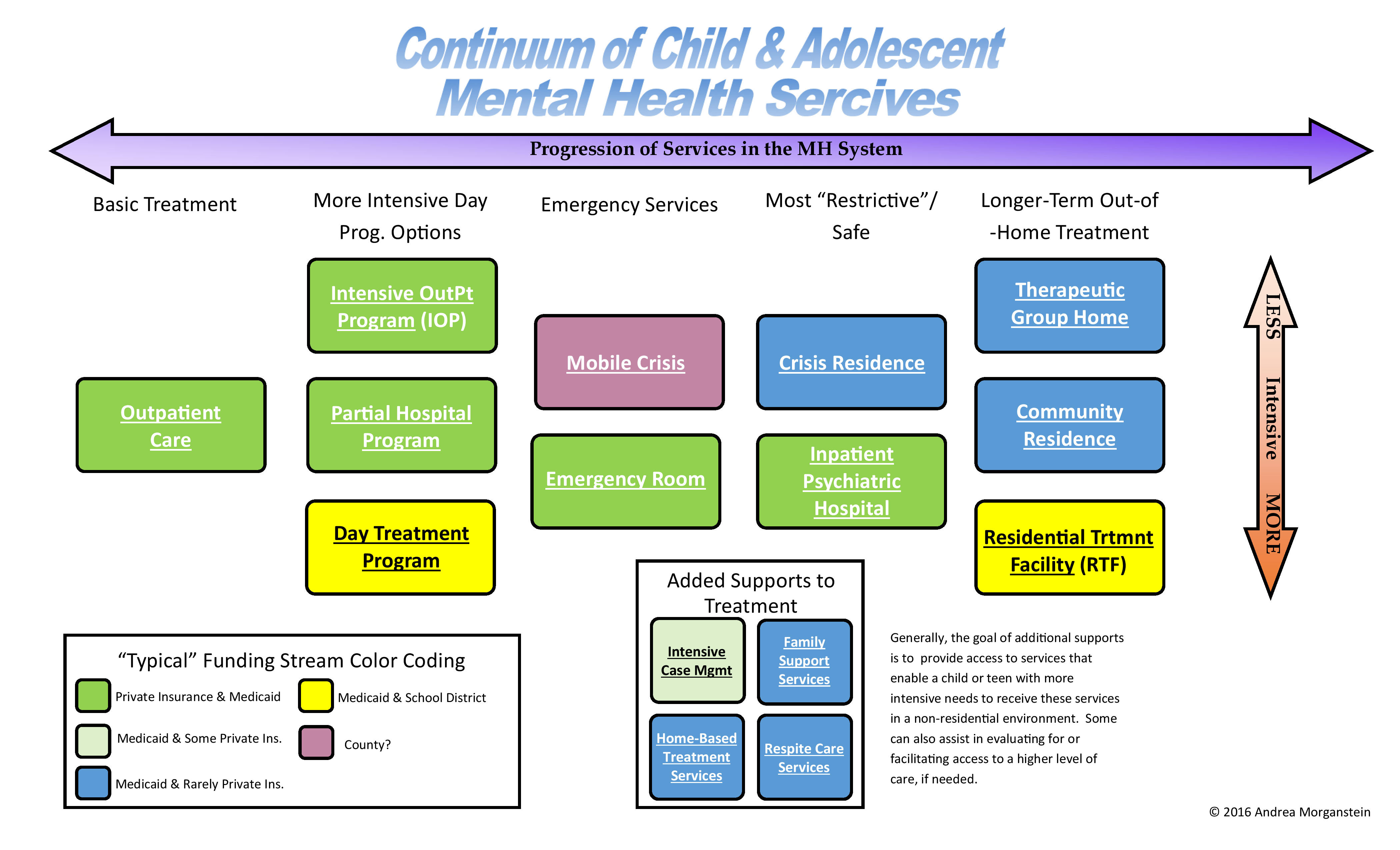
 The mental health system can feel overwhelming and complicated to people who are trying to navigate this system for the first time. Some people don’t need to know this information as outpatient therapy is the only involvement they ever have with the mental health system. But for children and teens who need more assistance than basic therapy, it can be very helpful to understand the different types of services that are available, what they’re called, and how they typically are paid for. The infographic below is designed to do just that.
The mental health system can feel overwhelming and complicated to people who are trying to navigate this system for the first time. Some people don’t need to know this information as outpatient therapy is the only involvement they ever have with the mental health system. But for children and teens who need more assistance than basic therapy, it can be very helpful to understand the different types of services that are available, what they’re called, and how they typically are paid for. The infographic below is designed to do just that.
I believe that all of these services exist in Philadelphia County and each county within the Philly suburbs. However, if you live in a different area, you would need to check to see which services are available in your county. A place that you might start is Google, using the key terms listed in the information below. Primary care physicians can be another resource and should be knowledgeable of, at least, the basics of what is available. Additionally, you can call the county’s mental health department for information. You might get passed around to a couple of different people before someone knows how to answer the question so you could start with something specific like, “Can you please tell me what agencies offer home based services in this are?”
The adult system has most, if not all of the services and levels of care that are listed below. There are also additional services that address employment and housing (and possibly more?) but I am less familiar with these additional services and how they relate to one another, at least at this time.
View as Color PDF |
View as B&W PDF |
The Effect of "Power Posing" Likely Depends on Context and Our Thoughts share
 I had mentioned Amy Cuddy’s work about power posing to a similarly scientifically-minded person recently and, after doing some reading on their own, they brought to my attention a blog article posted on the Scientific American website, The Dark Side of Power Posing: Cape or Kyrptonite, by Jay Van Bavel (11/212013). It took a look at Amy Cuddy’s work about ‘power posing’ and then pulled in some other relevant research findings. Basically, research suggests that there are traits within us and within our environment that affect whether power posing is helpful or makes things worse. One study found that, if you are a person who struggles with a lot of negative self-talk, power posing can actually have the opposite effect and decrease self-confidence. Other studies suggest that power posing can also be used to increase the likelihood of us doing things that amount to an abuse of power, such as: steal; cheat; or break traffic rules.
I had mentioned Amy Cuddy’s work about power posing to a similarly scientifically-minded person recently and, after doing some reading on their own, they brought to my attention a blog article posted on the Scientific American website, The Dark Side of Power Posing: Cape or Kyrptonite, by Jay Van Bavel (11/212013). It took a look at Amy Cuddy’s work about ‘power posing’ and then pulled in some other relevant research findings. Basically, research suggests that there are traits within us and within our environment that affect whether power posing is helpful or makes things worse. One study found that, if you are a person who struggles with a lot of negative self-talk, power posing can actually have the opposite effect and decrease self-confidence. Other studies suggest that power posing can also be used to increase the likelihood of us doing things that amount to an abuse of power, such as: steal; cheat; or break traffic rules.
I found Van Bavel’s article very interesting because, after I learned about Cuddy’s work, I had been curious about how it connects to the scientific research about the power of positive mental imagery. Research in the area of sports psychology has found a significant connection between athletes mentally rehearsing their craft and improvement in their ability to perform the tasks their sport requires. And trauma research has revealed that healing can take place when we re-imagine a traumatic event and role-play ourselves as powerful and able keep ourselves safe. So, after learning about how power posing affected body chemistry, I had wondered if simply imagining a power pose could shift body chemistry as well.
Because Van Bevel’s ‘Dark Side’ article is generally talking about the importance of our thoughts when we strike a pose, that what we are thinking affects whether we can use poser posing for ‘good’ or for ‘evil,’ it leads me to suspect that our body chemistry does change when we imagine ourselves doing a power pose. Hopefully, a researcher will take a look at that in the near future. More importantly, though, the notion that our thoughts can influence whether a power pose is a good thing, suggests to me that pairing the power pose with positive self-talk is critical so that we can increase the likelihood of using our power for the good of ourselves and for society in general. The next time you are doing your Wonder Woman pose before your next job interview, I would suggest that you are also imagining yourself speaking to the interviewer in a confident and personable way.
Executive Functioning Skills share
What are these skills you speak of?
 “Executive functioning skills” is a term that is used to describe our brain’s ability to plan, organize, and complete tasks. Brain functions such as short-term memory, mental flexibility, and self-control are all involved in these types of tasks. In your day to day life, this means that you are capable of developing strong executive functioning skills if your brain does well with remembering, being able to shift gears or “think outside of the box,” and being self-aware enough to enable you to control impulses and adjust your actions when change is helpful. If you are lucky enough to have strong executive functioning skills you will more easily develop the ability to:
“Executive functioning skills” is a term that is used to describe our brain’s ability to plan, organize, and complete tasks. Brain functions such as short-term memory, mental flexibility, and self-control are all involved in these types of tasks. In your day to day life, this means that you are capable of developing strong executive functioning skills if your brain does well with remembering, being able to shift gears or “think outside of the box,” and being self-aware enough to enable you to control impulses and adjust your actions when change is helpful. If you are lucky enough to have strong executive functioning skills you will more easily develop the ability to:
- Find things when you need them rather than spending half of your planned task activity just trying to locate the items that you need.
- Keep track of tasks that need to get taken care of or appointments/dates to keep instead of constantly needing to apologize for forgetting to do things or show up when you promised to.
- Prioritize things that are the most important over accomplishing other perhaps the easier ones…or the ones that are less tedious…or the ones that just happen to be in front of your face (I call these rabbit holes…a major weakness of mine, I go down rabbit holes all the time. My professional husband also uses the term, “project creep” when he is encouraging me to avoid it and stay on task. ).
- Chunk/plan out long term projects so that you can gather the necessary materials and then work on them gradually rather than leaving it all to the last minute.
- Estimate how long a task will take, fairly accurately, so that as you plan things in your schedule or on your “To Do” list, you have reasonable expectations of yourself rather than expecting yourself to have 8 hands and 2 brains and then feel like a failure when you don’t accomplish everything on your list.
Anxiety & Depression share
 Anxiety and depression affect a significant portion of our population: 18.1% of US adults had some form of excessive anxiety within a 12 month period in 2005 and 9.5% have some form of mood disorder.1 The numbers for a US adult having either of these two issues at some point within their lifetime is even higher: anxiety disorders, 28.8%; mood disorders, 20.8%.2 Genetics, how we were raised, poor nutrition/eating habits, lack of physical exercise, not enough sleep, use of drugs and alcohol, and life events can all play a role in why someone might struggle with anxiety and/or depression.
Anxiety and depression affect a significant portion of our population: 18.1% of US adults had some form of excessive anxiety within a 12 month period in 2005 and 9.5% have some form of mood disorder.1 The numbers for a US adult having either of these two issues at some point within their lifetime is even higher: anxiety disorders, 28.8%; mood disorders, 20.8%.2 Genetics, how we were raised, poor nutrition/eating habits, lack of physical exercise, not enough sleep, use of drugs and alcohol, and life events can all play a role in why someone might struggle with anxiety and/or depression.
Trying to eat three well-balanced, healthy meals (that include adequate protein and complex carbohydrates), getting adequate sleep (minimum 6-7 hours/night), regularly exercising (even if it’s just a 10 minute walk up the street and back), and avoiding use of drugs and alcohol can go a long way in helping to reduce the intense emotions you may be struggling with. Additionally, Cognitive Behavioral Therapy, and an newer off-shoot of it, Dialectal Behavioral Therapy, are two forms of therapy that scientific research shows to be quite effective in treating both anxiety and depression. (And, if there is underlying trauma that fuels the anxiety and/or depression, other types of therapy like EMDR, Brainspotting, Somatic Therapy, and Developmental Needs Meeting Strategy (DNMS) can really go a long way with helping the body come back to being able to feel safe and secure and significantly reliving the depression and anxiety symptoms.)
As this site continues to grow, you will find resources to help you better understand some of the struggles you are going through, to help you realize that you aren’t alone, and to find ideas about how you can move forward through the more challenging times in your life while reaching out to others friends and family (and/or therapist if you need) for support. Be sure to check out the How to Use This Site page to get you familiar with how resources are organized on the site. For those of you who would rather just jump in without an instruction manual, you can either search for key terms or move your mouse over Resource Index by Topic in the top menu bar and jump right in! The best place to start for issues based in anxiety or depression would be the Anxiety & Depression Index.
Sources:
1 Kessler Ronald C., et al. Prevalence, severity, and comorbidity of twelve-month DSM-IV disorders in the National Comorbidity Survey Replication (NCS-R). Archives of General Psychiatry, 2005 Jun;62(6):617-27.
2 Kessler, Ronald C., et al. “Lifetime prevalence and age-of-onset distributions of DSM-IV disorders in the National Comorbidity Survey Replication.” Archives of general psychiatry 62.6 (2005): 593-602